Alzheimer’s and vascular dementia: two paths of decline
When someone begins to experience memory loss and cognitive changes, it's often a frightening time for both the individual and their family. Two of the most common diagnoses are Alzheimer’s dementia and vascular dementia. While both result in cognitive decline, they stem from very different underlying causes. Understanding these differences is the first step toward appropriate diagnosis and care.
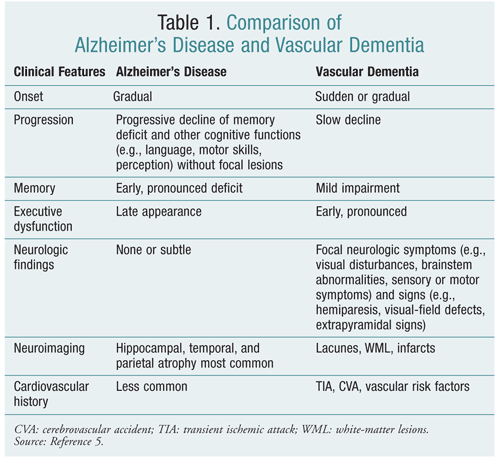
Alzheimer’s is primarily a neurodegenerative disease. This means it’s caused by the progressive damage and death of brain cells, largely due to the buildup of abnormal protein deposits—amyloid plaques and tau tangles. Vascular dementia, on the other hand, is typically caused by reduced blood flow to the brain. This can happen due to stroke, a series of small strokes, or other conditions that damage blood vessels.
These causes change how symptoms show up. Alzheimer’s usually creeps in slowly, starting with forgotten names or missed appointments. Vascular dementia often hits harder and faster, especially after a stroke, affecting how quickly someone thinks or makes decisions. The two often overlap, which makes a clear diagnosis difficult.
Early warning signs
The early symptoms of Alzheimer’s and vascular dementia can be subtle, and often mistaken for normal age-related changes. With Alzheimer’s, the hallmark sign is memory loss that disrupts daily life—forgetting recently learned information, repeatedly asking the same questions, or getting lost in familiar places. Difficulty planning or solving problems, confusion with time or place, and changes in personality or mood are also common.
Vascular dementia often presents differently. Because it's linked to blood flow issues, symptoms can appear more abruptly, potentially following a stroke or a series of "silent" strokes that go unnoticed. These can manifest as weakness or numbness on one side of the body, difficulty with balance, problems with executive functions like planning and organizing, and slowed thinking. It's not uncommon for someone with vascular dementia to have noticeable changes in gait or speech.
Symptoms often bleed into one another. You might see memory loss alongside a sudden struggle to organize a grocery list. Because of this blur, you need a professional evaluation rather than assuming it's just a normal part of aging. Catching it early gives you more time to adjust the home and plan for what's next.
New diagnostic tools
Diagnosing dementia accurately is a complex process. For years, diagnosis relied heavily on cognitive assessments and medical history. Now, we’re seeing exciting advancements in diagnostic tools that offer more objective evidence. In Alzheimer’s, PET scans that detect amyloid and tau proteins in the brain are becoming more widely available, though access and cost remain barriers for some.
Blood-based biomarkers are also rapidly evolving. The p-tau217 blood test, for example, shows promising results in identifying early Alzheimer’s pathology, even before symptoms appear. While not yet standard care, these tests are increasingly used in research settings and are expected to become more commonplace in clinical practice. However, interpreting these results requires expertise, and they aren’t foolproof.
For vascular dementia, improved neuroimaging techniques like MRI and CT scans are helping doctors assess blood flow and identify white matter lesions—areas of damage caused by reduced blood supply. Cognitive testing batteries are also becoming more sophisticated, designed to differentiate between the cognitive profiles of Alzheimer’s and vascular dementia. The goal is to move away from simply identifying that a dementia is present, to determining which dementia is driving the symptoms.
- Alzheimer’s: PET scans for amyloid and tau, plus p-tau217 blood tests.
- Vascular dementia: MRI and CT scans to find white matter damage.
Diagnostic Tool Comparison: Vascular Dementia vs. Alzheimer's Disease (2026 Outlook)
| Test Name | Alzheimer's Disease - Evidence Strength | Vascular Dementia - Evidence Strength | Relative Cost | Accessibility |
|---|---|---|---|---|
| PET Scan (Amyloid) | Better for: Detecting amyloid plaques, a hallmark of Alzheimer's | Limited Value: Amyloid presence doesn't directly indicate vascular dementia | Higher | Specialized Centers |
| PET Scan (Tau) | Better for: Identifying tau tangles and disease stage in Alzheimer's | Limited Value: Tau pathology is less directly linked to vascular dementia | Higher | Specialized Centers |
| Blood Biomarkers (p-tau217) | Promising: Emerging as a strong indicator of Alzheimer's pathology | Limited Value: Currently less established for vascular dementia diagnosis | Moderate | Increasingly Available |
| MRI | Good for: Assessing brain atrophy patterns consistent with Alzheimer's | Better for: Visualizing vascular damage (strokes, white matter lesions) characteristic of vascular dementia | Moderate | Widely Available |
| CT Scan | Useful for: Ruling out other causes, but less sensitive than MRI for early Alzheimer's changes | Good for: Identifying acute strokes and significant vascular changes | Lower | Widely Available |
| Cognitive Testing | Essential for: Establishing baseline cognitive function and tracking decline in both conditions | Essential for: Identifying specific cognitive deficits (executive function, processing speed) common in vascular dementia | Lower | Widely Available |
Qualitative comparison based on the article research brief. Confirm current product details in the official docs before making implementation choices.
Genetics and lifestyle risks
Genetics play a role in both Alzheimer’s and vascular dementia, but in different ways. For Alzheimer’s, the APOE4 gene is the most well-known genetic risk factor. Carrying one or two copies of this gene increases your risk of developing the disease, but it doesn’t guarantee you will. Many people with APOE4 never develop Alzheimer’s, and many without it do.
With vascular dementia, the genetic component is less direct. Instead, genetics can contribute to risk factors like high blood pressure or high cholesterol, which significantly increase the likelihood of developing the condition. This is where lifestyle choices become critical. Managing blood pressure, cholesterol, and blood sugar, quitting smoking, maintaining a healthy weight, and regular exercise can substantially reduce your risk.
It’s important to remember that genetics are complex, and lifestyle plays a huge role. You can’t change your genes, but you can control many of the factors that influence your risk of vascular dementia. Even for Alzheimer’s, a healthy lifestyle may help delay the onset or slow the progression of the disease.
Medication Management: Current and Emerging Therapies
Currently, medications for Alzheimer’s primarily focus on managing symptoms rather than curing the disease. Cholinesterase inhibitors (like donepezil and rivastigmine) and memantine can temporarily improve cognitive function, but their effects are modest and don’t halt the progression of the disease. Emerging therapies, like anti-amyloid antibodies (lecanemab and donanemab), offer a potential new approach, but they also come with risks and are not suitable for everyone.
Lecanemab, for example, has shown some ability to slow cognitive decline in early-stage Alzheimer’s, but it can cause side effects like brain swelling and bleeding. Donanemab has also demonstrated similar benefits in clinical trials. These medications are relatively new and require careful monitoring. Their long-term effects are still being studied.
For vascular dementia, the focus is on managing underlying cardiovascular risk factors. Medications to control blood pressure, cholesterol, and diabetes are crucial. There aren’t currently any medications specifically approved to treat vascular dementia itself, but managing these risk factors can slow the progression of cognitive decline. It's important to discuss all medication options and potential side effects with a doctor.
Support for Caregivers: Resources and Strategies
Caring for someone with dementia is incredibly demanding, both emotionally and physically. It’s essential for caregivers to prioritize their own well-being. Seeking support from family, friends, or support groups can make a huge difference. Remember, you can’t provide good care if you’re completely depleted.
Resources like the Alzheimer's Association and the National Institute on Aging offer support groups and research-based guides. You can also find practical caregiving tips at alzheimers.gov.
Practical strategies for caregivers include breaking down tasks into smaller, manageable steps, establishing a routine, and learning effective communication techniques. Don’t be afraid to ask for help, and remember that it’s okay to take breaks. Your health and well-being are just as important as the person you’re caring for.
Essential Tools for Navigating Vascular Dementia and Alzheimer's Care

Track items like keys, wallets, and luggage using Google's Find My Device network. · Features a 2-year battery life and IP65 waterproof rating. · Designed for Android users, compatible with Google's Find Hub App.
These tracker tags can help caregivers locate misplaced essential items, reducing stress and enhancing safety for individuals prone to wandering or misplacing belongings.

Provides 4 loud reminder alarms to prompt medication intake. · Features 14 large compartments for AM/PM doses over 7 days. · Moisture-proof design with a large screen for easy viewing.
This pill organizer ensures timely medication adherence with its loud alarms and ample compartments, crucial for managing complex treatment regimens in dementia care.

Offers large print, easy-to-follow coloring activities designed for seniors. · Aims to enhance memory, reduce stress, and improve mood through engaging art. · Activities are specifically tailored for individuals with dementia.
This coloring book provides a calming and mentally stimulating activity that can help improve mood, reduce anxiety, and engage cognitive functions in individuals with dementia.

Designed with tear-away snaps for easy and discreet dressing and undressing. · Features open-back and shoulder snaps for convenient post-surgery access. · Made from soft, adaptive fabric for comfort.
These adaptive gowns offer comfort and dignity while simplifying the dressing process for individuals with limited mobility or those recovering from surgery, easing caregiving tasks.

A comprehensive guide for families caring for individuals with Alzheimer's and related dementias. · Offers practical advice on daily care, communication, and managing challenging behaviors. · Covers a wide range of topics relevant to memory loss in later life.
This essential guide provides invaluable, in-depth knowledge and practical strategies for caregivers navigating the complexities of dementia care, supporting both the individual and their family.
As an Amazon Associate I earn from qualifying purchases. Prices may vary.




No comments yet. Be the first to share your thoughts!