Vascular dementia after the pandemic
Families are seeing more dementia cases since the pandemic, often appearing earlier than expected. This isn't just anecdotal; doctors are tracking a rise in vascular dementia diagnoses linked to post-viral complications.
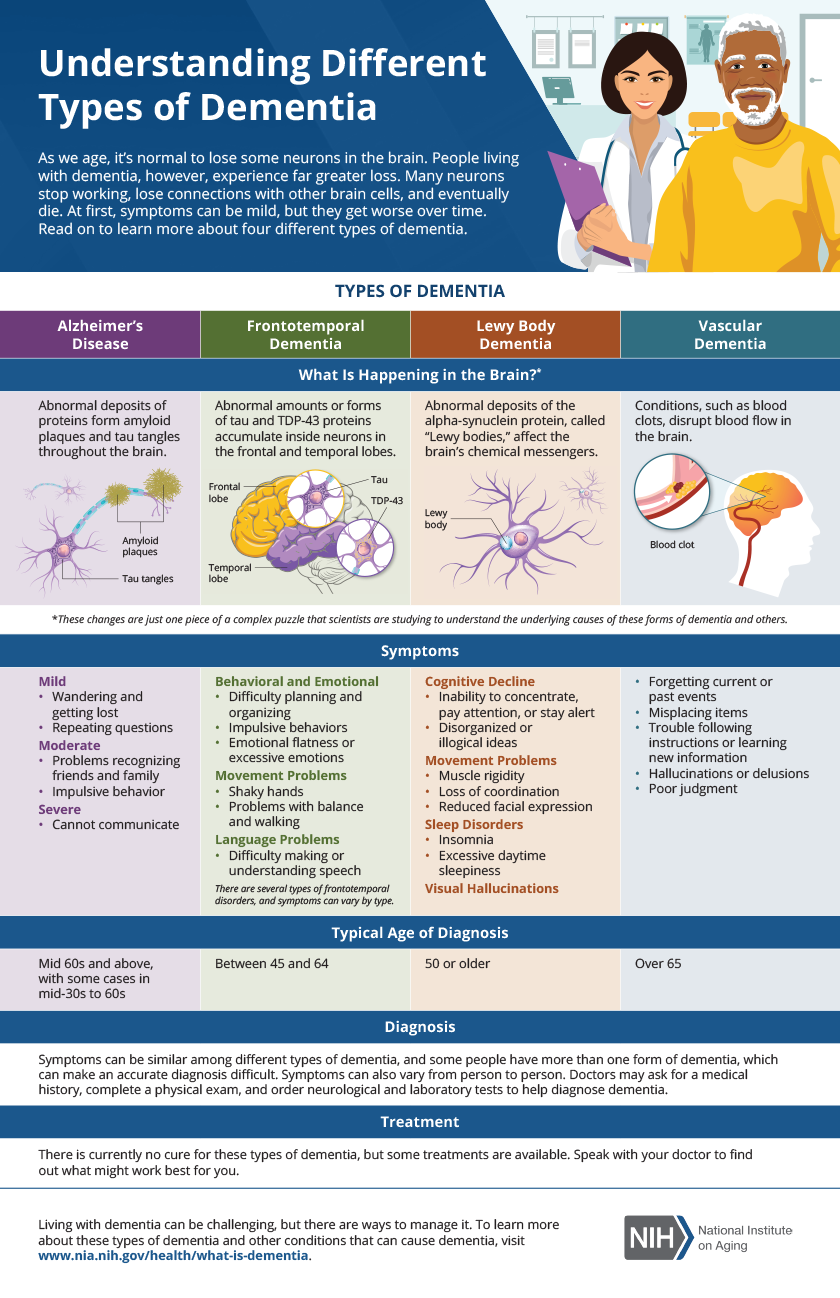
Vascular dementia is not a single disease, but rather a group of conditions caused by reduced blood flow to the brain. This can happen due to strokes, or smaller, less obvious damage to blood vessels. It’s different from Alzheimer’s disease, which is characterized by specific protein deposits in the brain. While both cause cognitive decline, the way that decline happens often differs.
A 2023 study in The Lancet found a spike in dementia diagnoses within 12 months of a COVID-19 infection. While we don't know the full long-term effects yet, the connection is strong enough that families should plan for higher vascular risks after a severe bout with the virus.
I want to be upfront: we’re still learning. The data is complex, and the long-term effects of COVID-19 are still unfolding. But acknowledging the potential connection is the first step in preparing families and advocating for better research and support.
How the virus affects the brain
COVID-19 can impact brain health in multiple ways, all of which can contribute to the development of vascular dementia. One key mechanism is inflammation. The virus triggers a systemic inflammatory response, and this inflammation can cross the blood-brain barrier, causing damage to brain cells and blood vessels.
Another significant concern is the increased risk of blood clots associated with COVID-19. These clots can block blood flow to the brain, leading to stroke – a major cause of vascular dementia. Even in individuals who experience mild COVID-19 cases, microclots can form, subtly restricting blood flow over time. This chronic reduction in blood supply can lead to gradual cognitive decline.
The virus can also directly damage the endothelial cells that line blood vessels in the brain. This damage impairs the blood vessels’ ability to function properly, further reducing blood flow and potentially leading to stroke or other vascular problems. It’s not just severe cases, either; even mild infections can have lasting neurological consequences.
Long COVID often brings brain fog and fatigue that doesn't go away. These aren't just temporary annoyances; they are signs of cognitive strain that require a medical evaluation to rule out permanent vascular damage.
Symptoms to watch for
The symptoms of vascular dementia can be subtle and often overlap with other conditions, making diagnosis challenging. Unlike Alzheimer’s, which often presents with gradual memory loss, vascular dementia frequently manifests as a "step-wise" decline – periods of relative stability followed by sudden declines in cognitive function. These declines often coincide with mini-strokes or other vascular events.
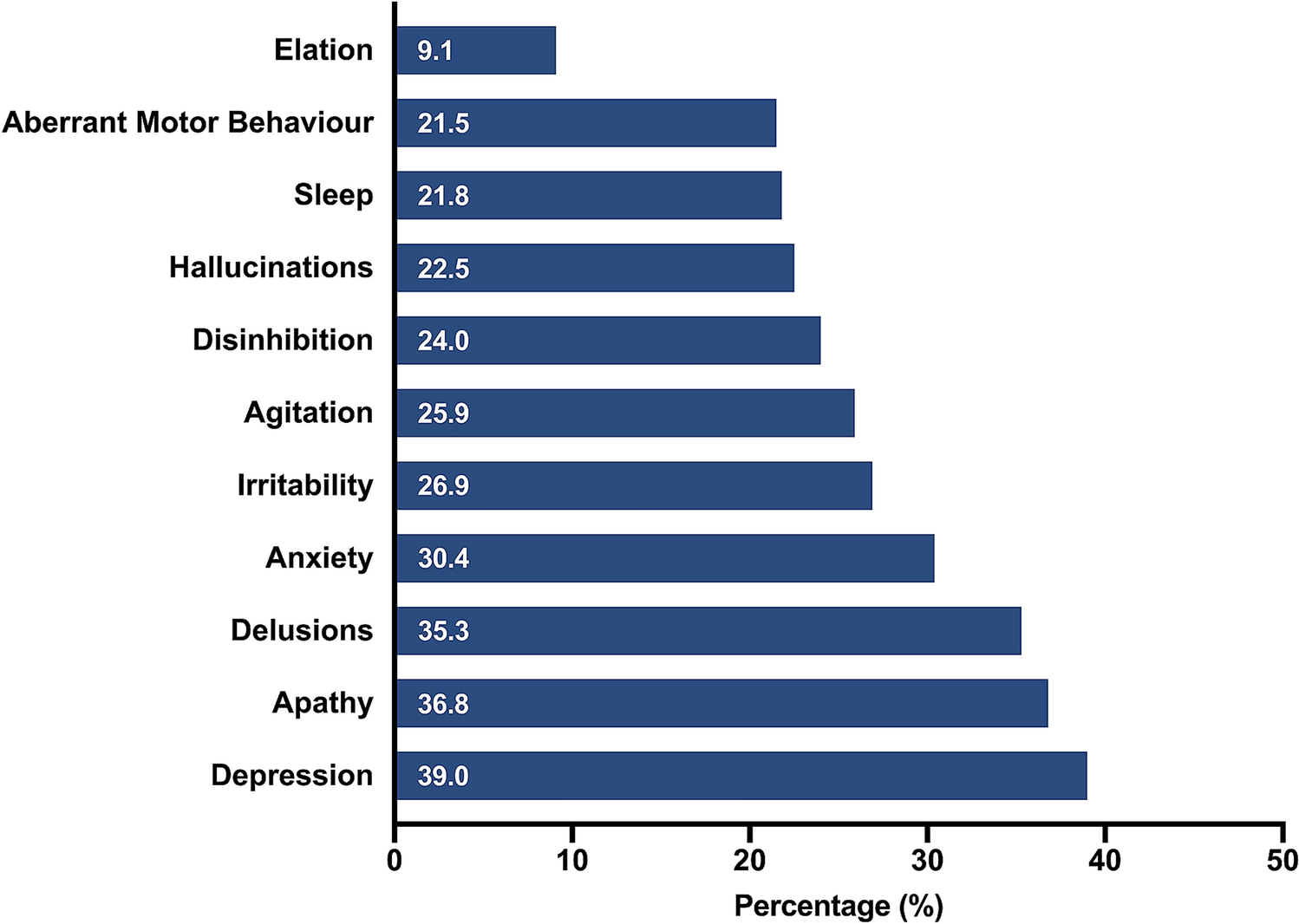
Mood swings are also more prominent in vascular dementia than in Alzheimer’s. Individuals may experience periods of depression, anxiety, or irritability. Changes in personality are common, and they can be quite disruptive. Look for sudden shifts in behavior or emotional reactivity.
A key difference is the potential for focal neurological signs. These are symptoms that affect specific areas of the brain, such as weakness on one side of the body, difficulty with speech, or problems with balance. These signs suggest damage to specific blood vessels in the brain, rather than the diffuse damage seen in Alzheimer’s.
Early detection is critical. If you notice any of these symptoms, it’s important to seek a thorough medical evaluation. Don’t dismiss changes as simply "getting older." Distinguishing vascular dementia from other conditions, like depression or medication side effects, requires careful assessment by a healthcare professional.
Diagnosis in 2026
Diagnosing vascular dementia involves a comprehensive assessment, typically starting with a medical history and physical exam. Your doctor will likely ask about your loved one's symptoms, medical history, and any medications they're taking.
Neuroimaging plays a crucial role. MRI and CT scans can help identify evidence of strokes, white matter damage, and other vascular changes in the brain. Cognitive assessments, such as the Mini-Mental State Examination (MMSE) or the Montreal Cognitive Assessment (MoCA), are used to evaluate cognitive function.
Neuropsychological testing provides a more detailed assessment of specific cognitive domains, such as memory, attention, and executive function. This testing can help determine the pattern of cognitive impairment and differentiate vascular dementia from other types of dementia. Expect a detailed, multi-hour evaluation.
Research is ongoing to identify biomarkers – measurable indicators of disease – that could aid in earlier and more accurate diagnosis. Blood tests and cerebrospinal fluid analysis are being investigated, but these are not yet widely available in clinical practice. While we aren’t promising a quick fix, the field is actively pursuing new diagnostic tools.
Caregiving strategies
Caring for someone with vascular dementia can be challenging, but with the right strategies, you can improve their quality of life and your own. The unpredictable nature of the symptoms is often a significant hurdle. Be prepared for fluctuations in cognitive function and adjust your expectations accordingly.
Communication is key. Speak clearly and slowly, using simple language. Avoid complex sentences or abstract concepts. Repeat information as needed, and be patient. Nonverbal communication – eye contact, touch, and a calm demeanor – can be particularly helpful. The National Institute on Aging (nia.nih.gov) offers excellent resources on effective communication techniques.
Creating a safe environment is essential. Remove tripping hazards, install grab bars in the bathroom, and ensure adequate lighting. Consider a medical alert system in case of falls or emergencies. Managing medications is also critical. Work with your doctor to create a medication schedule and ensure adherence.
Behavioral changes, such as agitation or aggression, can be distressing. Try to identify triggers and address them proactively. Redirect the individual's attention, offer reassurance, and avoid confrontation. Remember to prioritize your own well-being. Caregiving is demanding, and you need to take time for yourself to rest and recharge. Explore resources from alzheimers.gov for caregiver support.
Research and prevention
Ongoing research is focused on understanding the underlying causes of vascular dementia and developing new treatments. Scientists are investigating potential therapies to protect blood vessels, reduce inflammation, and promote brain health.
Lifestyle factors play a significant role in preventing vascular dementia. Controlling blood pressure, managing cholesterol, maintaining a healthy weight, and getting regular exercise can all reduce your risk. A heart-healthy diet, rich in fruits, vegetables, and whole grains, is also beneficial.
While there’s no guaranteed way to prevent vascular dementia, adopting these healthy habits can significantly lower your risk. Researchers are also exploring the potential of new drugs and therapies to prevent or delay the onset of the disease.
I want to end on a note of empowerment. Encourage families to advocate for their loved ones, participate in research studies, and stay informed about the latest advances in dementia care. By working together, we can improve the lives of those affected by this challenging condition.


No comments yet. Be the first to share your thoughts!